Could Polio Outbreak Put Kids at Risk? State Vaccination & Exemption Rates Vary
Get stories like this delivered straight to your inbox. Sign up for The 74 Newsletter
Amid the ongoing COVID-19 pandemic and the accompanying debate over vaccines, an old virus is threatening to reemerge: polio.
Earlier this month, the virus was detected in the United States for the first time since 2013. An unvaccinated man in New York tested positive for poliomyelitis, the scientific name for the illness; where he contracted it is still unclear.
Although the last case that originated in the U.S. occurred in 1979, unvaccinated people are at risk. Vaccine hesitancy and missed doctor’s appointments because of COVID-19 mean some kids aren’t getting the protection physicians say they need.
The Centers for Disease Control and Prevention recommends children receive four doses of the polio vaccine between 2 months and 4 years old, and schools and child care facilities in every state require the shots, which are safe and effective, before children can attend. But around the United States, vaccination rates vary widely.
Every state allows children to be exempted from the immunizations for medical reasons. Washington, D.C., and 44 states allow religious exemptions, and 15 allow philosophical exemptions, according to the National Conference of State Legislatures.
Within a state, vaccination coverage can vary widely as well. In Rockland County, New York, for example, where the first case of 2022 was detected, about 60% of residents over age 2 are vaccinated, according to recent state data. In Nearby New York City, where the virus has been detected in wastewater, the overall rate is about 86%. Even within the city, rates differ, with some neighborhoods reaching higher than 99% while others are as low as about 56%.
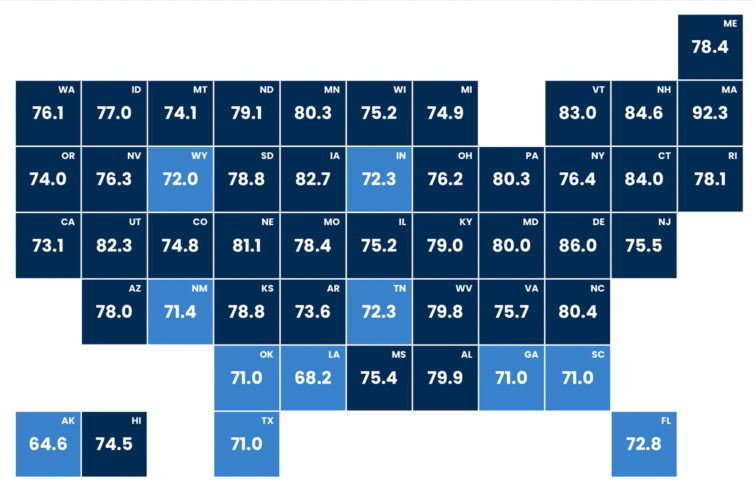
The map below shows the share of toddlers in each state who received the recommended series of vaccines — which includes immunization against polio as well as measles, mumps, rubella, varicella and other illnesses — by 35 months old.
Share of Children Who Have Received Recommended Series of Vaccines by 35 Months
Graphic by Eamonn Fitzmaurice/The 74
For herd immunity from polio, about 80% of people in a community need to be immunized, according to the World Health Organization. The vaccination rate associated with herd immunity — the minimum share of people who must be protected to stop an illness from spreading— varies by disease.
Polio is often asymptomatic but can cause flu-like symptoms. In rare cases, the virus can result in muscle weakness, paralysis or death. Anyone who is not vaccinated can contract polio, but it most commonly affects children under 5 years old, according to the World Health Organization.
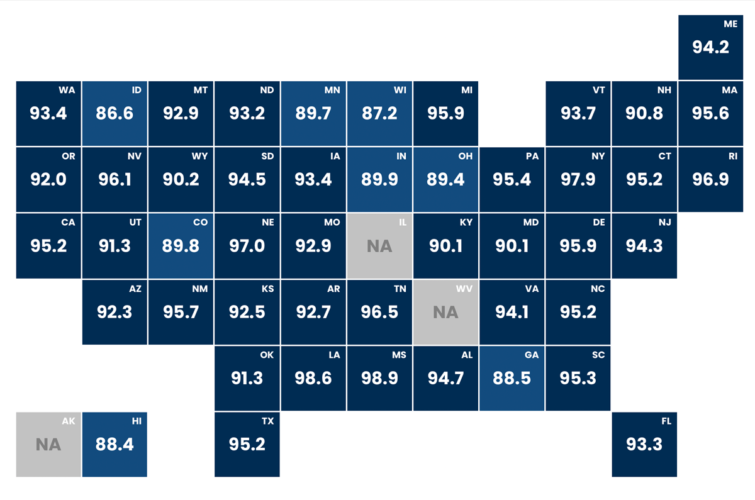
This map shows the percentage of kindergartners in each state who have received the recommended doses of the polio vaccine.
Share of Kindergarteners Vaccinated Against Polio By State
Graphic by Eamonn Fitzmaurice/The 74
In the early 1950s, before the vaccine was available, polio caused “more than 15,000 cases of paralysis each year,” according to the CDC. Schools played a vital role in vaccine trials in the later part of that decade.
One reason vaccines are less popular than they were when polio was widespread is because they work, David Oshinsky, a medical historian at New York University and the author of Polio: An American Story, told NPR last year.
Effective vaccines have “obliterated evidence of what [polio] can cause: kids on crutches, in wheelchairs, in iron lungs,” he said. “I remember seeing the occasional empty desk in school because a child had died. People had seen polio every summer, and they wanted kids vaccinated as soon as possible.”
Get stories like these delivered straight to your inbox. Sign up for The 74 Newsletter

;)
