Naloxone in Schools: Why School Nurses Are Jumping Into the Fight Against Heroin Overdoses
Wearing a dinosaur T-shirt, a 4-year-old boy sat in the back seat, staring blankly into the camera. Privacy issues aside, the viral photo released by an Ohio police department in September offered a literal snapshot of America’s devastating opioid epidemic — a problem that frequently begins with a prescription for painkillers and often ends in death.
The young boy in the photo was an innocent bystander in a plague that took more than 28,000 American lives in 2014, according to the Centers for Disease Control and Prevention — triple the total in 2000. Abuse is most prevalent among adults, but school-age children are also taking opioids, including prescription painkillers and heroin, at alarming rates.

In 2014, nearly half a million young people between the ages of 12 and 17 used opioid pain medications without a prescription, and an estimated 28,000 used heroin.
As overdoses continue to grab headlines, school nurses have joined the fight against abuse — though firm evidence about the prevalence of overdoses in schools doesn’t yet exist.
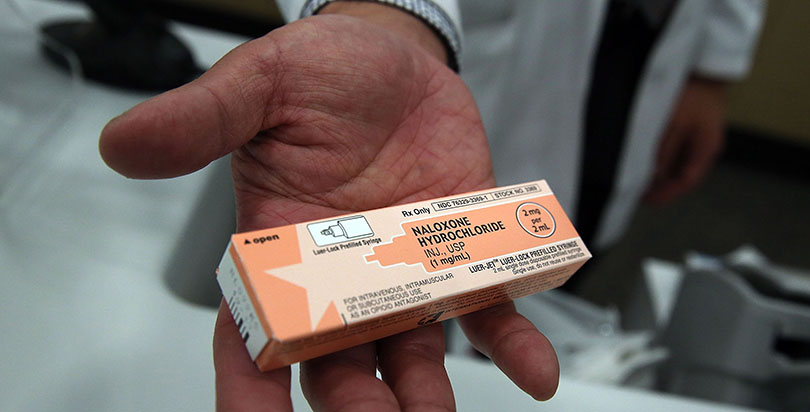
Non-prescription opioid use among teens is on a downward trend, according to a 2015 report by the National Institutes of Health, and heroin use — typically lower among teens than other substances — is at an all-time low. Still, nurses are often first responders in school emergencies, so the National Association of School Nurses (NASN) is calling on education officials across the country to buy naloxone, the antidote to heroin and opioid overdose also known by its trademarked name, Narcan, and to train school staff how to use it.
Districts in heroin hotbeds like Ohio and Pennsylvania have already begun to stock their school medicine cabinets with naloxone.
In New York, Gov. Andrew Cuomo announced last year that the state would spend nearly $300,000 to put naloxone kits in schools and to train staff in their use, an effort that he said would “go a long way toward saving young lives.”
Of the five states that adopted laws last year to place naloxone in schools, Rhode Island was possibly the most aggressive, requiring it in all public schools. That law followed a state survey of school nurses, nearly half of whom reported students in their schools were using opioids.
In September, the NASN released a toolkit calling for more state legislators and school district leaders to jump on board, supported by a grant from the company that makes Narcan Nasal Spray. The toolkit, which can be downloaded on the association’s website, includes information on different types of naloxone, a sample naloxone policy for school districts, training tips for school staff and a presentation for officials who hope to secure the antidote for their schools.
“Part of school nursing is surveillance, so you’re always looking in your community to see what might be coming,” said Rebecca King, a school nurse in Delaware who has helped lead an advocacy effort to stock Narcan in schools. “We don’t like it when it comes, but when it comes we man up, we get resources, and we’re ready to fight whatever it is that comes along.”
As a mother — and a nurse for nearly two decades — King is acutely aware of opioid abuse. It’s a disease that almost killed her daughter.
Only two weeks into her first semester at the University of Delaware, King’s daughter Stephanie, who is now 27, was sexually assaulted, and a doctor prescribed Percocet tablets for her stomach pains. She became addicted, and it wasn’t long before she switched to heroin — which was cheaper and easier to get — and became trapped in a raging addiction.
After a while, she wasn’t using heroin to get high, a euphoric feeling that one Reddit user described as “being cradled to sleep by God.” She used so she didn’t feel sick.
Stephanie overdosed twice but lived, and after a tough road through rehab, she recovered. She went back to college and became a recovery coach for a local counseling group.
“I wish I knew all about this back when my daughter was first using,” King said. “I wish somebody would have told me what the signs of that addiction looked like.”
Though Stephanie became addicted in college, not in high school, her experience gave her mother a new sense of urgency about the possibility of overdoses among younger students. Although little evidence exists that students are overdosing on opioids in school, King argues that is because schools are reluctant to share firsthand accounts.
King helped shepherd state legislation in 2015 that placed naloxone in Delaware schools, but she hasn’t heard of schools officials in Delaware, or anywhere in the U.S., who have needed to use it. Rather, she said, her emphasis is on prevention, if an emergency were to occur.
Matt Ruth, the U.S. chief commercial officer for Adapt Pharma, agrees. Adapt Pharma partnered with the Clinton Foundation in January to offer all public schools a free two-dose box of Narcan Nasal Spray. With a two-year expiration date, the box otherwise would cost $75. The drug doesn’t have any side effects if it’s used on someone who isn’t overdosing, he said.
Acknowledging that overdoses aren’t frequent on high school campuses, he said the company offered the product to educate school officials and students about opioid use. Educators in Pennsylvania, New Hampshire, Massachusetts, Kentucky and Ohio have accepted the drug from Adapt Pharma.
“It’s not as easy to give away this type of potentially lifesaving product as you might think, and that’s disappointing,” Ruth said. “However, we feel like by making the offer, we hope to cause a disruptive conversation to occur, and to start a conversation, and maybe more and more people will become educated and will ultimately take us up on our offer.”
Even if naloxone hasn’t been used in schools, media reports suggest that first responders have administered the drug to teens. In October, for example, paramedics in Pennsylvania resuscitated a 16-year-old with four hits of naloxone when she overdosed on heroin she had gotten from her father. And a student at Pennsylvania’s Brandywine Heights Area High School was rushed to the hospital when she overdosed on heroin at the beginning of the school day. School officials didn’t respond to requests for comment.
“Some superintendents and principals, they’re kind of like, ‘What is this? We don’t have this problem here, so why do we need this?’ that kind of thing, so it’s really up to the nurses to educate the community,” King said. “We’re first responders, too. We’re first responders in the school setting.”
Correction: A previous version of this article incorrectly stated that Stephanie King, who attends college, had graduated.
Get stories like these delivered straight to your inbox. Sign up for The 74 Newsletter

;)
